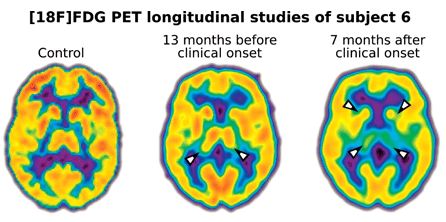
PET with fluorodeoxyglucose as pre-symptomatic FFI diagnostic
 Read with caution! This post was written during early stages of trying to understand a complex scientific problem, and we didn't get everything right. The original author no longer endorses the content of this post. It is being left online for historical reasons, but read at your own risk. |
In recent posts on amyloid plaque imaging and BLI & MRI biomarkers, I wrote that it seemed no one had figured out a good marker to use in PET scans for as a diagnostic or an early biomarker for prion disease. I may have spoken too soon. A few recent studies have found that glucose metabolism appears to be reduced in certain parts of the brain in GSS [Kepe 2010], CJD [Renard 2008, Kim 2012] and FFI [Cortelli 2006]. Glucose metabolism can be imaged using fluorodeoxyglucose radiolabeled with 18F. This molecule is a glucose analog, so it gets taken up and retained by cells that are metabolizing glucose. So if you see less signal than expected (based on controls) in a particular brain region, that means you may be seeing reduced glucose metabolism there.
Cortelli’s study followed FFI carriers and controls for 10 years and looked at rCLMglc (regional cerebral metabolic rate of glucose) across the brain via PET scanning with fluorodeoxyglucose. Four of the carriers became symptomatic during the 10 year interval, and the three who were imaged all showed a 30-40% reduction in glucose metabolism in the thalamus during the disease course. One also showed smaller ~20% reductions in glucose metabolism in the limbic cortex and basal ganglia. One of these four individuals had been imaged 13 months before any symptoms were noted and had already shown about a 16% reduction in glucose metabolism in the thalamus. No one else was imaged that close to disease onset; one person imaged 21 months before disease onset showed no changes. Though it’s a sample size of one, the authors suggest that reductions in glucose metabolism probably start between 21 and 13 months before symptoms. So this could potentially be an early biomarker.
This reduction in metabolism could be due to impairment of neurons, or to loss of some neurons. The authors cite evidence from other neurodegenerative diseases, mostly Alzheimer’s, suggesting that impaired glucose metabolism occurs before neuronal loss begins, so the reduction observed might just be due to prions starting to impair the cells’ function.
Subject 6, who had the abnormal PET scan 13 months before onset, also had some subtle abnormalities in sleep EEG at that same follow-up visit, though it sounds like the authors didn’t notice it until re-examining the data retrospectively.